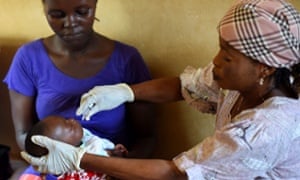
 When I met members of a women’s secret society in Sierra Leone this February, they proposed drastic measures to stop Ebola from spreading through sexual contact. All survivors should be quarantined for three months, they said. Male survivors need to be locked up because they cannot control their urge to have sex. Women need to be locked up because they cannot stop their husbands from forcing sex upon them. When I asked them whether using condoms might be easier than quarantine, I was greeted with rolling eyes and hissing. Their men would never accept this. “They would put holes in the condoms as soon as they saw them”. Female condoms? Forget it. “They are disgusting. They get stuck deep into women’s body.”
When I met members of a women’s secret society in Sierra Leone this February, they proposed drastic measures to stop Ebola from spreading through sexual contact. All survivors should be quarantined for three months, they said. Male survivors need to be locked up because they cannot control their urge to have sex. Women need to be locked up because they cannot stop their husbands from forcing sex upon them. When I asked them whether using condoms might be easier than quarantine, I was greeted with rolling eyes and hissing. Their men would never accept this. “They would put holes in the condoms as soon as they saw them”. Female condoms? Forget it. “They are disgusting. They get stuck deep into women’s body.”
These responses suggest that international health organisations’ official recommendations for preventing the transmission of Ebola through sexual contact, which advise survivors returning from treatment centres to use condoms or refrain from sex, are not being adhered to. global development professionals
Join the Guardian Global Development Professionals Network
Join up to access commentary and insight from development experts across the world.
Click here
Being clear about how Ebola is spread is vital. According to the World Health Organisation, “men who have recovered from the illness can still spread the virus to their partner through their semen for up to seven weeks after recovery”. The view of the Centers for Disease Control and Prevention (CDC) is that sexual transmission of Ebola has not been definitively established, but it agrees that “multiple studies have shown the Ebola virus can persist in semen for longer than in blood or other body fluids”. As my meeting with the women’s secret society made clear, contradictory communication on Ebola as a sexually transmitted disease leaves people to come up with their own preventive methods.
Women’s secret societies are ancient cultural institutions found all over Sierra Leone. They teach Sierra Leonean girls to become women through a comprehensive hands-on curriculum which includes sex education. Outsiders lack detailed knowledge of these rituals. But secret societies have become notorious for conducting female genital mutilation (FGM) as part of this education during “Bondu” rituals.
Given the secret societies’ poor reputation on sexual and reproductive health, it would be easy to dismiss their idea of a three-month quarantine as another “traditional” erroneous belief. But the behaviour-change messages from international NGOs, on how to prevent Ebola spreading through sexual contact, are confusing and maladapted to local gender inequities.
Advertisement
Abstinence-based sexual messages are problematic because people have sex – voluntary and involuntary – for lots of reasons. That’s not going to stop because of Ebola. Sierra Leone has one of the highest maternal mortality rates in the world, which is closely related to the high prevalence of teenage pregnancies. More than a quarter (26%) of girls aged 15-19 have already given birth, and 40% of all maternal deaths are teenage pregnancies. Billboards all over the country encourage girls to stay in school and not get pregnant, but without sex education and access to contraceptives this has been idealistic.
The summer holiday is locally well known as a period when schoolgirls get pregnant. Schools have been closed since last summer, prolonging this high-risk period to almost nine months. There is little to do for young, curious people. Sexual abstinence messages are not likely to work when unmarried teenagers lack access to both contraceptives and safe-sex negotiation skills.
Moreover, poor girls may be engaged in transactional sex. Travel restrictions have prevented people from working, planting and trading for many months, causing hunger and a depletion of already scarce resources. Farmers have had to eat their own seeds to survive. They have had to stay at home while their tools and harvests were rotting on their land. Without traders, both quarantined and non-quarantined households in quarantined villages cannot not buy food. In this context it is not unlikely that girls will exchange sex for food or other basic needs more than during a normal school holiday.
Before Ebola, when teenagers became pregnant – by choice or by force – they entered a weak primary health care system that focused on maternal and child health rather than safe sex and the prevention of unwanted teenage pregnancies. During this outbreak, however, young people have been left even more to their own sexual devices than before. In a few months, girl’s bodies will show us the results.
On the other hand, many lessons have been learned during the Ebola outbreak. There’s been an increase in knowledge, skills and, in some cases, access to water, sanitation and hygiene (Wash) through extensive collaboration with national and international government and non-governmental organisations. Wells have been rehabilitated, buckets and soap donated, and handwashing campaigns have been run. Teachers and students have been especially important in leading these efforts.
Unplanned pregnancy is only one of the sexual and reproductive health issues keeping girls out of school. Lack of Wash facilities for menstruating girls is another. Reinforcing Ebola-related Wash benefits in schools could therefore have positive gender, sexual and reproductive health effects post-Ebola.
Teachers and students will soon be going back to school, but pregnant girls will not be joining them due to a new ruling by the ministry of education. They are seen as bad examples for other students. This is discriminating and stigmatising. It aggravates the vulnerability of women and girls who are just coming out of a particularly difficult period in their lives because of Ebola.
If we want to strengthen Ebola prevention during the tail-end of the outbreak we should focus our efforts on getting gender-sensitive wash facilities in schools to prevent new infections among students. We can chose to focus on improving sexual and sexual reproductive health – or we can choose to give people health messages so ill-adapted to their lives that they roll their eyes at us and hiss.
GUARDIAN (UK)
END

Be the first to comment